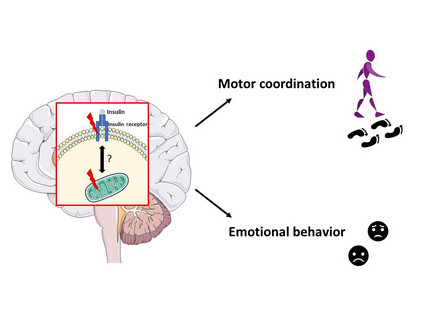
Project 2: Impact of brain insulin action on mood and motor coordination
Diabetes and insulin resistance are associated with altered cognition, motor coordination and mood. Patients suffering from diabetes and insulin resistance are at increased risk for depression or anxiety disorders. Conversely, patients with depression also exhibit an increased risk to suffer from diabetes. In some cases, depression can lead to poor compliance to follow a therapy regime or even suicide. Thus, understanding the molecular links between diet-induced cerebral insulin resistance and emotional alterations is of paramount importance. Yet, the relationship between obesity, diabetes, insulin resistance and emotional disorders is poorly understood.
Here, we investigate consequences of altered insulin action and emotional behavior. To assess this, we use the technique of intranasal insulin application to specifically affect brain function and behavior while avoiding peripheral consequences of excessive insulin signaling. Moreover, we analyze the effect of novel modulators of brain insulin signaling with respect to emotional behavior.
Furthermore, brain insulin resistance is associated with Parkinson disease (PD). In some studies, diabetic patients exhibit a 40 % higher risk of developing PD and insulin sensitizers are currently used in a clinical study to treat PD. PD patients exhibit features of altered insulin signalling with reduced expression of insulin and IGF-1 receptors and further downstream signalling molecules. In addition, both diseases share common dysregulated pathways such as neuroinflammation, oxidative stress and mitochondrial dysfunction. Loss of insulin sensitive, dopaminergic neurons in the substantia nigra is a hallmark of PD.
In this project , we aim to understand the contribution of a diminished insulin-regulated mitochondrial function for the development of PD, as a common mediator for the potential development of metabolic and neurodegenerative diseases.